This post may contain affiliate links. If you click through a link and make a purchase, I may receive a commission at no additional cost to you. As an Amazon Associate, I earn from qualifying purchases. Read the full disclosure here.
Knowing what to avoid when you’re dealing with Achilles tendon pain is just as important to get you feeling better fast.
In this article, I’ll review five exercises to avoid with Achilles tendonitis to stop the roller coaster ride of symptom exacerbation so you can start feeling better.
Disclaimer: This content is for educational purposes and is not medical advice. Read the full disclaimer.
Exercises to avoid with Achilles tendonitis
Friendly reminder, this doesn’t mean “avoid these exercises for life,” this only means they may not be the best choice with an inflamed Achilles tendon and could contribute to worsening symptoms.
Smart physical activity modification is important for getting better, balancing gentle movement without overdoing it.
A proper rehab program includes building these activities back in when appropriate to gradually get the tissues used to various demands again.
Related read: Why Does My Achilles Tendon Feel Tight? (14 Potential Causes)
1. Aggressive stretching
Tight calf muscles are a common complaint with Achilles tendonitis.
Wanting to stretch is a natural reaction; however, aggressive stretching can tug at the Achilles insertion and worsen symptoms. “Aggressive stretching” means things like stretching too much, pulling too hard, or bouncing while stretching.
Constant stretching may worsen the issue if this area is already irritated, including a delayed pain response to stretching. Not to mention, Achilles tendonitis may give you the perception of your calves feeling tight, even if they aren’t. Flexibility is part of recovering from Achilles pain, but it isn’t the only part.
One of my favorite ways to stretch the calves is by using an adjustable calf stretch board. These boards have adjustable angles to accommodate to your current flexibility needs and provide a comfortable amount of stretch.
The StrongTek Professional Wooden Slant Board is well-made with stretch angles ranging from 15 degrees all the way up to 35 degrees.
Related read: How To Stretch Tight Calves
2. Incline walking or running
The calf muscles help propel us forward when walking or running. Walking or running up inclines causes these muscles/tendons to work harder through a larger range of motion. This can cause additional Achilles pain to an already irritated area.
Training errors are a common cause of overuse injuries. Rapid increases changes in terrain, such as adding hills into your walking or running routine, can contribute to overuse and Achilles tendonitis.
Stick with flat surfaces until you get the green light to progress, and then build inclines slowly back into your routine.
3. Jumping (Plyometrics)
Plyometric training (aka jump training or “plyos”) is a method to improve strength, power, and reactive movements.
Plyometrics involve an eccentric muscle contraction followed by an explosive concentric contraction, such as jumping onto a box or surface.
Plyometrics place a lot of strain on tissues, so it’s best to avoid this type of training if you’re dealing with any Achilles tendon pain. Plyometric training appears in the later phases of Achilles tendonitis treatment when the tissues are ready to tolerate this type of load and demand.
4. Sprinting
Sprinting involves short bursts of high-intensity running and is often used in interval training for both runners and workouts such as HIIT workouts.
Adding too much sprinting too quickly into an exercise or running program may result in Achilles tendonitis. Be sure to add program changes gradually to give the tissues of the body time to accommodate to new training modalities.
Since sprinting involves maximal effort, this may be too much demand on an injured Achilles tendon.
5. Certain sports
Modify or avoid any sports with components of running, cutting, jumping, inclines, or being on the toes for an extended period (such as ballet).
In the meantime, you can focus on strength training or other fundamental skills of the sport.
What is Achilles tendonitis?
The Achilles tendon is the thickest and strongest tendon of the human body. It’s made of thick fibrous connective tissue that connects the calf muscles (at the back of the lower leg) to the heel so we can do things like walk, run, and jump.
Tendons have a unique function to store and release elastic energy to make our movement more efficient and reduce the work required by muscles.
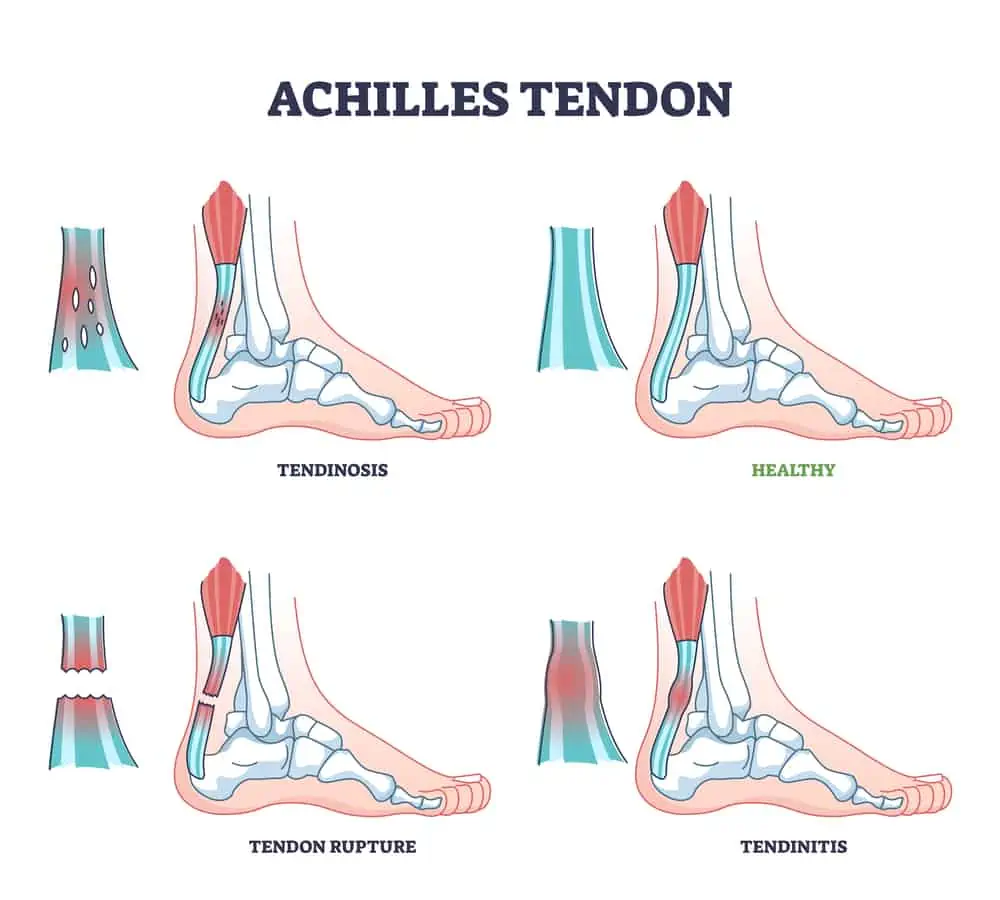
Achilles tendonitis (tendinitis, tendinosis, or tendinopathy) is an overuse injury or irritation of the Achilles tendon. Tendonitis refers to more acute inflammation, and tendinopathy or tendinosis is more chronic in nature.
Symptoms of Achilles tendinopathy include pain and stiffness (especially in the morning, after sitting for long periods of time, or after exercise) at the point where the tendon inserts into the heel bone (insertional Achilles tendonitis) or further up the tendon.
Other noteworthy signs may be tenderness to touch or swelling, difficulty rising up on your toes, or pushing off during walking or running.
Achilles tendonitis tends to be more common in men, runners, or those who are ”weekend warriors” (as in being mostly sedentary during the week and saving all of your enthusiasm for the weekends).
There’s also an increased risk for Achilles tendon injury with certain antibiotics or corticosteroid use.
An Achilles tendon rupture is either a partial or full tear of the Achilles.
How to fix Achilles tendonitis
We’ve focused on what to avoid that makes Achilles tendonitis worse; now, let’s talk about some things that can help an Achilles injury.
When you’re dealing with an injured tendon, simply resting doesn’t fix problems and often provides a false sense of pain relief, leading to a longer period of time before someone gets their pain addressed.
Another trap that people often fall into is using tape, straps, or other passive treatments but then continuing with the same bad habits that brought on the issue in the first place.
A healthy balance of activity modification and proper exercise is the best combination to feel better.
Here are some tips to approach your rehab for success:
- DO get evaluated to determine the cause of your pain and set you up with the proper exercise program for you.
- DO pay attention to your symptoms so you can articulate them to your health care providers to receive a more specific treatment.
- DO learn about your condition so you can better understand safe ways to move and avoid exacerbations.
- DO be consistent with your prescribed home program.
- DO speak up and problem solve with your healthcare providers when something isn’t working.
- DO manage your expectations for healing and celebrate small wins toward getting back to normal.
When to see a doctor
Here are some reasons why you might want to see an orthopedist or even a foot/ankle specialist for your Achilles pain.
- New or sudden onset pain, swelling, or weakness
- Inability to rise on your toes or push off while walking
- You feel a divot or lump in the tendon
- You’ve tried all the conservative treatments, and nothing seems to be working
You can also try physical therapy if there are no immediate red flags (such as a sudden loss in plantar flexion strength). A physical therapist can evaluate you for not-so-obvious underlying causes of your pain.
Many states now have direct access to physical therapy, allowing you to go directly to a physical therapist without a prescription.
You may need to follow up with your doctor within 30 days (varies by state) to continue PT, but this allows you to access rehab services faster.
It may also depend on the particulars of your insurance plan. Call your local PT office for information specific to your area.
If you’ve never had physical therapy before, don’t miss this article outlining how to prepare for your first appointment and where you can get a free checklist!
Wrapping up
Achilles tendon pain can range from mildly annoying to debilitating.
Understanding what to avoid and proper rehabilitation strategies are important for reaching your goals and feeling better.
References
Gabbett TJ. The training—injury prevention paradox: should athletes be training smarter and harder? British Journal of Sports Medicine 2016;50:273-280.
Roberts TJ, Konow N. How tendons buffer energy dissipation by muscle. Exerc Sport Sci Rev. 2013 Oct;41(4):186-93. doi: 10.1097/JES.0b013e3182a4e6d5. PMID: 23873133; PMCID: PMC3836820.