This post may contain affiliate links. If you click through a link and make a purchase, I may receive a commission at no additional cost to you. As an Amazon Associate, I earn from qualifying purchases. Read the full disclosure here.
Plantar heel pain is a very common overuse injury and has a reputation for being tricky to relieve.
Many times, I find that patients are unknowingly doing many of these things that can secretly make your plantar fasciitis worse.
Learning what not to do with plantar fasciitis can help you stop the cycle of making your pain worse and finally start making progress toward getting better.
Disclaimer: This content is for educational purposes and is not medical advice. Read the full disclaimer.
Disclaimer: This content is for educational purposes and is not medical advice. Read the full disclaimer.
What not to do with plantar fasciitis
Are these habits making your plantar fasciitis pain worse? Let’s learn the do’s and don’ts for plantar fasciitis.
Here’s a detailed list of things to avoid when you have plantar fasciitis so you can start feeling better faster.
Avoid high impact activities
The plantar fascia helps to support the natural arches of the foot, helping to properly transfer load and force throughout the body. Different activities increase the tensile force on the plantar fascia at different rates and can be uncomfortable for the already irritated tissue.
Running and jumping increases the forces throughout the body. Depending on the intensity of the exercise, forces have been measured anywhere between two and ten times your body weight at various joints.
Even your running style and whether you strike with your forefoot (front of the foot) or rear foot (heel strike) affects the stress through the plantar fascia.
Instead, choose low-impact activities while your plantar fascia is healing to avoid taking one step forward and two steps back. To keep moving with less stress to your injury, check out this list of low-impact workouts that are joint-friendly.
Related read: 8 Low-Impact Alternatives To Running
Avoid spending too much time on your feet
Of course, moving throughout the day is encouraged, but spending too much time on your feet when you have plantar fasciitis can make it more difficult for your body to heal.
If standing and walking are a must for your job, invest in some supportive footwear and insoles or possibly try and anti-fatigue mat to help alleviate lower leg discomfort.
On your breaks, try to give your feet a rest and work in some easy stretches.
Avoid unsupportive footwear
Unsupportive footwear such as flip-flops, ballet flats, and slip-on shoes can contribute to plantar fasciitis. Even expensive casual shoes can be unsupportive.
Always choose supportive shoes that fit properly if you know you’ll be standing and walking for extended periods.
If you already have plantar fasciitis, stay away from these types of footwear until your symptoms resolve. When you go back to wearing these types of shoes, choose wisely based on activity demands.
Brooks makes some of the best sneakers on the market and features several different styles to suit different types of feet. I’m a huge fan of the Glycerin line.
If it’s summertime and you’re looking for supportive sandals, check out Birkenstock and Fitflop. Both of these brands have plenty of support for your foot over the average flat flip-flop.
Get 20% off your order at Fitflop here.
Related read: Are Birkenstocks Good For Plantar Fasciitis?
Invest in good quality shoes
Cheap shoes are made from low-quality materials which break down quickly. Higher quality materials have better support and last longer under daily demands.
Some well-known high-quality shoe brands are:
The price tag on good quality footwear may be a turn off. However, you’re not really saving any money if you have to keep replacing poor-quality shoes at more frequent intervals.
If you’re looking to save money on sneakers, you can always try searching for previous models of the shoe. Many companies will put older models on sale once the new model is released.
Also, don’t be swayed by cozy words like “cloud” and “memory foam” insoles. These materials typically wear out very quickly and leave you unsupported.
Also, do your research if shopping at outlet stores. Sometimes you can score big deals on high-quality shoes that are just last year’s model. Other times, outlet shoes are lower quality and made specifically for the outlet, so you’re not really getting as much of a deal as you think.
Related reads:
Avoid aggressive stretching of the foot and ankle
Stretching the calves and feet is often a recommended part of recovering from plantar fasciitis. But stretching too aggressively can irritate the plantar fascia and render your stretching session counterproductive.
For best results, aim for the feeling of tension and pulling, but not pain. Then gently hold and breathe for 20-30 seconds until you feel the area start to loosen up.
With stretching, less tends to be more.
To learn a variety of foot and ankle stretches, read this.
Avoid focusing only on the foot
A common misconception with plantar fasciitis is that focusing on the area of pain will eventually heal your symptoms.
In reality, the body is all connected, and other areas that seem unrelated can change the way you move, causing foot pain, and leading to conditions such as plantar fasciitis and Achilles tendonitis.
Many other areas of the body, including restrictions in foot and ankle joints, hip extension, and even hip muscle weakness, can be contributors to plantar fasciitis.
A thorough movement assessment by a physical therapist can help identify other areas that may be contributing to your foot pain and design a well-rounded treatment approach.
To read more about these surprising causes in-depth and what you can do to improve your pain, read this article.
Avoid pushing through the pain
Pushing through musculoskeletal pain often leads to more pain, and potentially more areas involved as the body naturally begins to create abnormal movement patterns to compensate for the pain.
Activity modification is an important strategy in recovering from any orthopedic injury and is not the same as activity avoidance.
An important distinction is that modification doesn’t mean rest. Modification means adjusting time, technique, or intensity or activity to keep moving but avoid exacerbation (worsening) of your symptoms.
This is where that annoying 1-10 pain scale comes in handy.
Rate your pain on the scale and be honest with yourself; you’re not competing with anyone. When your pain starts to rise 2-3 points above that initial rating, it’s probably time to take a break before the pain gets severe.
Your progress will be faster if you can avoid aggravating your symptoms frequently.
Avoid the “set it and forget it” approach
What I mean by this is making no other changes and relying on some type of passive “fix” like an arch support, heel wrap, or taping.
Sure, these things may have a place in your rehab, but passive tools shouldn’t be the only thing you’re relying on because they don’t permanently fix issues.
Tissues of the body need to be loaded, moved through full range of motion, and strengthened to see lasting improvement. Movement is medicine, and a more active approach can help you fix bad habits that lead you to pain in the first place, instead of just placing a bandaid over the larger issue.
Avoid being sedentary
Rest alone does not tend to fix musculoskeletal issues. Rest may feel better temporarily, but upon returning to activity, the injured tissue isn’t prepared to handle loads, and the pain returns.
Intermittent rest with activity modification, along with progressive loading of tissues, helps to restore function.
In general, lack of exercise and movement increase your chances of being overweight and cause the weakening of muscles, tendons, and ligaments from disuse.
This can turn into a spiral of pain and sedentary behavior, significantly limiting overall mobility and quality of life.
Related read: How To Be More Active When You Hate Exercise
What is plantar fasciitis?
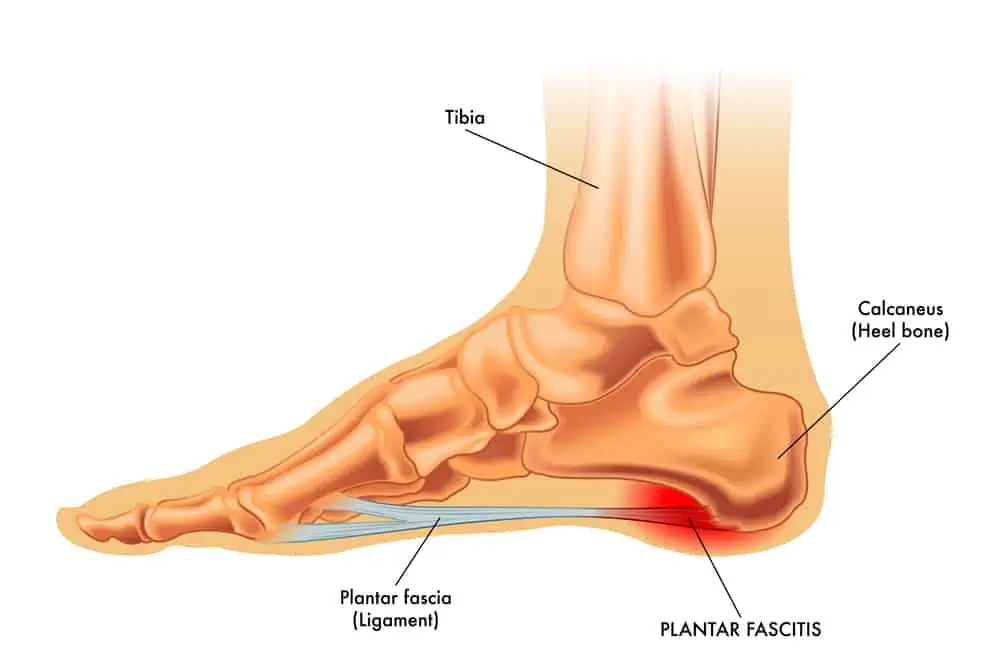
The plantar fascia is a thick band of connective tissue that runs along the arch of the foot to the heel bone. It functions to support the arch and transfer force through the foot and lower leg during movement.
When the plantar fascia ligament is asked to pull more than its fair share, it’ll let you know, in the form of severe pain with every step.
Plantar fasciitis is an inflammation of the fascia at its insertion point on the heel. If the pain becomes chronic, for example, for months to years, the condition may be called plantar fasciosis.
There’s also some newer evidence that chronic plantar fasciitis is related to decreased blood flow, which affects the body’s ability to get fresh blood carrying oxygen and other reparative cells to the area to initiate tissue healing.
This finding argues that chronic cases are less about inflammation and more about tissue degeneration, making the condition more multifactorial than originally thought.
Best tools to tackle plantar fasciitis pain
Here are some popular tools for home to address plantar fasciitis pain. When used properly and in conjunction with a well-rounded approach, they can be very helpful.
Scraping tools
Fascia scraping is a technique used to improve blood flow, decrease pain, improve mobility, and improve range of motion. The best part is that it’s easy to perform scraping on your own.
The best way to approach scraping for plantar fasciitis is to target the arch of the foot and the calf muscles.
Calf muscle tightness is a common contributor to plantar fascia pain, and combining scraping with targeted flexibility and strengthening exercises helps build a well-rounded approach for recovery.
As far as research goes, Xu Q et al. found that scraping can improve blood flow and tissue temperature to promote local blood circulation and energy metabolism.
My favorite tools for fascia scraping are from Sidekick tool, you can check them out here.
To read more about fascia scraping for plantar fasciitis, read this article.
Calf stretch board
My favorite way to do these stretches is with a slant board. I really feel like I get a great stretch whenever I use one. It’s always a crowd favorite in the physical therapy clinic too.
A slant board can be adjusted to provide different levels of intensity based on your flexibility. With a slant board, it’s easier to relax your calf muscles and use gravity to settle into a deep stretch.
This slant board on Amazon has an adjustable height, so you can change the level as your flexibility improves.
Orthotics & Insoles
Custom orthotics and over-the-counter insoles can be a great option along the plantar fasciitis journey.
An orthotic supports the foot’s arch, which also positively affects the alignment of other joints of the body from the ground up.
If you have particular needs, you will need to see a podiatrist for custom orthotics. The downside is they can be costly (in the neighborhood of $400-$600 per pair). Insurance limits how many pairs you can have, if they cover them at all.
For over-the-counter affordable, high-quality insoles, I recommend Superfeet.
They offer different types of insoles for all activities and are cost-effective enough to have several pairs to go around in your shoe collection.
An over-the-counter heel cup may also provide some much-needed plantar fasciitis relief. A silicone heel pad can provide extra cushioning and support to cradle a painful heel and decrease pain.
Night splint
A night splint is a frequently used tool for plantar fasciitis and Achilles pain.
During the night, the feet relax into more of a pointed (plantarflexed) position, and this shortens the plantar fascia tissue. This is one of the mechanical reasons why those first few steps in the morning tend to be so painful.
The goal of a night splint is to keep the affected foot in a more neutral position to maintain tissue length while you’re not on your feet to reduce pain and promote healing.
Research suggests that the use of a night splint may provide earlier relief of plantar fascia symptoms.
The downside is that it’s obviously not comfortable to sleep with a large boot contraption on your foot, and if you’re not getting quality sleep, then that will have an effect on your pain and healing as well.
Here are a few options on Amazon to try:
- BraceAbility Sleep Brace for plantar fasciitis
- United Ortho Plantar Fasciitis Support Brace
- WYX Plantar Fasciitis splint
What happens if plantar fasciitis is left untreated?
When plantar heel pain is left untreated, it can lead to chronic pain, plantar fascia tears, and heel spurs.
If you’ve had the pain for more than a few weeks, you likely can’t “walk it off.” Unresolved foot pain can also lead to the development of ankle, knee, hip, and back pain due to compensations in movement.
Conservative treatment can be very successful in treating plantar fasciitis symptoms. A physical therapist can help you learn the proper exercises and stretches for pain relief.
Related read: Does Physical Therapy Work?
Wrapping Up
Plantar fasciitis is well known for being painful and tricky to treat, leading people to suffer from these symptoms for quite a long time.
A multi-pronged approach is the best way to tackle plantar fasciitis from all angles.
Be sure to check out Surprising Reasons Why Your Plantar Fasciitis Isn’t Getting Better for a deeper look into other areas of the body that contribute to foot pain.
References
Cleather DJ, Goodwin JE, Bull AM. Hip and knee joint loading during vertical jumping and push jerking. Clin Biomech (Bristol, Avon). 2013 Jan;28(1):98-103. doi: 10.1016/j.clinbiomech.2012.10.006. Epub 2012 Nov 10. PMID: 23146164; PMCID: PMC3966561.
Miller LE, Latt DL. Chronic Plantar Fasciitis is Mediated by Local Hemodynamics: Implications for Emerging Therapies. N Am J Med Sci. 2015 Jan;7(1):1-5. doi: 10.4103/1947-2714.150080. PMID: 25709971; PMCID: PMC4325390.
Wheeler PC. The addition of a tension night splint to a structured home rehabilitation programme in patients with chronic plantar fasciitis does not lead to significant additional benefits in either pain, function or flexibility: a single-blinded randomised controlled trial. BMJ Open Sport Exerc Med. 2017 Jun 13;3(1):e000234. doi: 10.1136/bmjsem-2017-000234. PMID: 29259809; PMCID: PMC5731230.
Xu QY, Yang JS, Zhu B, Yang L, Wang YY, Gao XY. The effects of scraping therapy on local temperature and blood perfusion volume in healthy subjects. Evid Based Complement Alternat Med. 2012;2012:490292. doi: 10.1155/2012/490292. Epub 2012 May 14. PMID: 22666292; PMCID: PMC3359830.