This post may contain affiliate links. If you click through a link and make a purchase, I may receive a commission at no additional cost to you. As an Amazon Associate, I earn from qualifying purchases. Read the full disclosure here.
Not sure if you should be using ice or heat for neck pain?
That’s understandable. It’s quite a hot topic.
In fact, It’s one of the most commonly asked questions when someone first comes into physical therapy.
The wrong choice could increase discomfort, not to mention the annoyance of wasting time when all you want to do is start feeling better.
Let’s clear up all the confusion today, including everything you need to know about both modalities to choose the right one at the right time.
Disclaimer: This content is for educational purposes and is not medical advice. Read the full disclaimer.
Benefits of ice for neck pain
The thought of wrapping a freezing cold ice pack around an already stiff neck may sound like a torture session, however, ice has many benefits that may help address pain in the short term.
Superficial cold therapy can come in the form of ice packs, ice cubes, or cold water immersion/ice baths (although that’s not really for neck pain relief).
Using ice for an injury can:
- Constrict blood vessels
- Decrease circulation
- Decrease swelling
- Decrease pain, muscle spasm, or itching
Blood vessels respond to temperature changes. Ice constricts blood vessels and decreases circulation. This process can help to limit swelling in acute injuries.
The other major attraction to ice is pain reduction. The cold reduces nerve activity and is a localized, non-drug way to help manage pain following an injury.

When should you use ice?
Generally, ice is recommended immediately following a new injury and in the first few days after.
After that, you can still use ice as a form of pain management, but its effects on swelling are most significant immediately after injury.
If you’ve Googled around a bit, you may have come across some articles claiming ice is terrible, and we should stop using it.
Ironically, there isn’t much evidence that ice does much for healing. It’s just something we do. So I can’t fault people for wanting to dig deeper.
But people love to cherry-pick which evidence to follow to fit the narrative, no matter what side of the argument.
There’s been a big anti-ice movement (on the internet at least), with many claiming that ice impedes the body’s ability to heal.
The reasoning behind this is based on the theory that swelling brings blood flow and inflammatory mediator cells to clean up the mess and get you started on healing.
While inflammation may bring some additional pain, it’s also a necessary part of the healing process. By constricting blood vessels and limiting the signals, the healing process could take longer.
But what does that mean in the grand scheme? (And to us mere mortal non-professional athletes?)
There also seems to be a lack of evidence in humans comparing healing times with ice vs. no ice.
But we do know that bringing movement back to injured tissues (as soon as appropriate) helps the rehab process progress. (More on this in a bit.)
Psychologically, if a few minutes of ice decreases your pain and makes you more confident to get moving, isn’t that a positive thing? Especially since movement avoidance can lead to chronic neck pain.
Some moderation with ice is probably the winner here.
We likely don’t need to spend all day rotating ice packs for 20 min on and 20 min off, but a little cold to take the edge off and get you moving can be beneficial.
Here’s another article that dives deep into this argument if you’re looking to learn more.
Best ice packs for neck pain
No more dinky drug store ice packs that barely cover an injured area. Check out these high-quality ice therapy options.
My favorite ice packs are the Torex Mojility. The gel material inside this cold pack remains pliable even when frozen and easily molds to any body part.
Chattanooga Col Pac is also very good and what you typically find in a physical therapy clinic.
Both of these brands can stand up to a lot of use and come in various oversized dimensions.
The cervical size is great for your neck and a convenient option to wrap around ankles, knees, elbows, shoulders, and the neck. The other sizes are great for covering larger areas of the body.
Benefits of heat for neck pain
Superficial heat feels oh-so-cozy and can come from a microwave or water bath hot pack, heating pad, hot bath, or sauna.
- Increases blood flow
- Decreases feelings of pain, soreness, stiffness, and tight muscles
Because heat can increase blood flow by dilating blood vessels, it has the potential to increase swelling, which may cause additional discomfort.
Liquids can also move easier in warm temperatures than cold temperatures.

When should I use heat on an injury?
Heat can be used for injuries that didn’t happen today (or sometimes, in the past few days).
Reach for heat with general stiffness, soreness, or pain that isn’t associated with an acute injury.
Putting heat on an acute injury could make you feel much worse later on and increase your swelling.
Best heat packs for neck pain
I like this microwavable heat pack because it has a soft fabric strap to comfortably secure it around your back, neck, or shoulder.
You can also find full-length heat packs to cover larger areas, like the full back.
If you don’t want to deal with putting hot packs in the microwave, you can also check out electric heating pad options. This type of hot pack comes in a variety of sizes and allows you to adjust the temperature for comfort.
Precautions using ice and heat
Both ice and heat can cause damage if applied incorrectly. Here are some tips to make sure you stay safe with each.
- Always use buffer layers in between your skin and the ice/heat pack
- Limit usage to 10-20 min at a time
- Check the skin every few minutes
- Don’t fall asleep using ice or heat
- Use extra layers between you and the ice/heat if you’re lying on top of the pack
- Caution using in areas with decreased sensation or with people who have impaired cognition
- Avoid heat over open wounds, stitches, or swelling
- Caution with circulation problems
Ice or heat for neck pain – the fine print
Both of these modalities can be helpful, but it’s important to distinguish what they can and can’t do.
While both ice and heat packs may help you decrease pain, remember that these modalities are passive.
Using passive modalities only will not fix pain or injuries. They can be helpful for temporary pain management, but applying ice for weeks and doing nothing else won’t help you heal.
R.I.C.E (Rest, Ice, Compression, Elevation) is still circulating widely as a treatment for injuries, even though it dates back to the late 1970s.
This approach can still be appropriate in very acute phases; however, it sends the message that more rest and icing will get you better.
If you’re sitting around on an ice pack waiting to be 100%, I have bad news.
Only “ricing” will prolong your rehab.
After an initial acute phase, it’s essential to work your way back to normal activities gradually. This includes improving range of motion, strength and gradually loading your tissues again.
The latest proposed acronym for injuries to hit the streets is PEACE & LOVE.
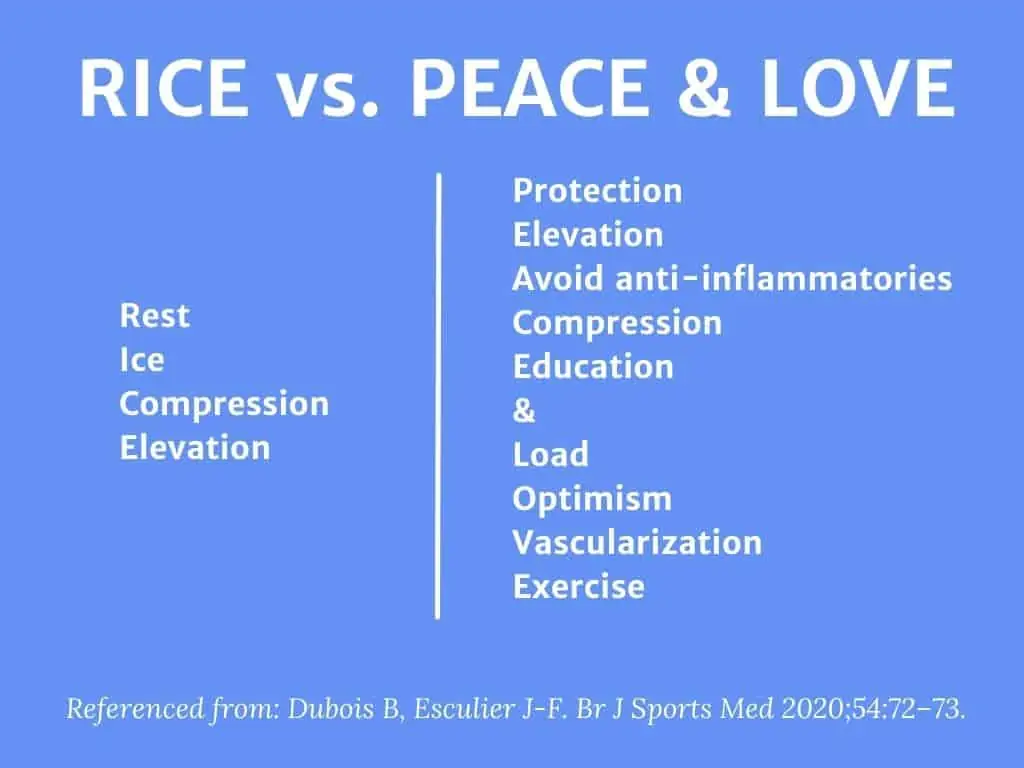
2020;54:72–73.
Although PEACE & LOVE advocates for avoiding ice, I think it outlines a more complete rehab picture from start to finish.
Tissue healing does take time and can be longer for complex injuries.
Make sure you have the guidance of a physical therapist to help you with an appropriate program.
What about topical cold/heat creams?
In the first aid aisle, you can also find an abundance of creams, gels, lotions, and potions to make an area hot or cold.
Wintergreen or menthol are often ingredients used to make you feel cold. Capsaicin is a common ingredient in heat creams.
All these over-the-counter examples are topical, meaning you’re just putting them on the outer layer of your skin, and they don’t penetrate very deeply (despite cleverly worded marketing claims).
The topical effect of hot or cold can provide temporary pain relief, but there isn’t anything magical that makes you better.
*Be sure not to use these at the same time as ice or heat, as they can impair your ability to judge temperature and put you at risk for a burn or other skin irritation.*
Also, always wash your hands after application.
The active ingredients are not something you want in your eyes, nose, or anywhere else.
Wrapping up
A neck problem is no fun and can really limit your overall activity tolerance.
It takes a long time for research to make it into regular practice and even longer for information to become mainstream. As we research and learn more, recommendations change over time.
Ice and heat are still widely popular, especially among athletes.
Is ice or heat better for neck pain? Both hot and cold therapy can help alleviate pain and make you more comfortable, whether it’s rehab or pain management.
In general, ice is better for new injuries or significant pain. Heat may feel more comfortable for chronic pain or stiffness.
If you’re still not sure which is best for you, check in with your healthcare provider.
When it comes to ice vs. heat for injuries, use passive modalities sparingly and be sure to follow rehab guidelines for your best outcomes.
References:
Dubois B, Esculier J-F. Soft tissue injuries simply need peace and love. Br J Sports Med 2020;54:72–73.
Freiwald J, Magni A, Fanlo-Mazas P, et al. A Role for Superficial Heat Therapy in the Management of Non-Specific, Mild-to-Moderate Low Back Pain in Current Clinical Practice: A Narrative Review. Life (Basel). 2021;11(8):780. Published 2021 Aug 2. doi:10.3390/life11080780
Petrofsky, Jerrold S.1; Khowailed, Iman Akef2; Lee, Haneul3; Berk, Lee1; Bains, Gurinder S.1; Akerkar, Siddhesh1; Shah, Jinal1; Al-Dabbak, Fuad1; Laymon, Mike S.4 Cold Vs. Heat After Exercise—Is There a Clear Winner for Muscle Soreness, Journal of Strength and Conditioning Research: November 2015 – Volume 29 – Issue 11 – p 3245-3252
doi: 10.1519/JSC.0000000000001127
Wang ZR, Ni GX. Is it time to put traditional cold therapy in rehabilitation of soft-tissue injuries out to pasture?. World J Clin Cases. 2021;9(17):4116-4122. doi:10.12998/wjcc.v9.i17.4116
White, G.E., Wells, G.D. Cold-water immersion and other forms of cryotherapy: physiological changes potentially affecting recovery from high-intensity exercise. Extrem Physiol Med 2, 26 (2013). https://doi.org/10.1186/2046-7648-2-26






Thanks for clearing up some of the confusion around the ice vs heat topic. As someone who’s had plenty of injuries (tendon tears), I’ve always wondered in what order I should apply things after an injury and during recovery. This helps.
Thanks for reading!