This post may contain affiliate links. If you click through a link and make a purchase, I may receive a commission at no additional cost to you. As an Amazon Associate, I earn from qualifying purchases. Read the full disclosure here.
When you have lower back pain, it’s a natural instinct to want to get some imaging to “see inside” and try to figure out what’s going on.
Many patients are quick to request an MRI for back pain and are discouraged when their provider won’t do a scan right away.
As a physical therapist, I hear this frustration frequently, so let’s explore when this imaging test is useful information and when it’s not, so you can be more confident in your treatment plan to get better fast.
Disclaimer: This content is for educational purposes and is not medical advice. Read the full disclaimer.
What is an MRI?
Magnetic resonance imaging (MRI) is a type of diagnostic imaging that uses a strong magnetic field along with computer-generated radio waves to create detailed pictures of the organs and tissues in your body.
MRI is a noninvasive method for your doctor to examine your insides. An MRI can produce high-resolution images of the inside of the body that help diagnose a variety of issues.
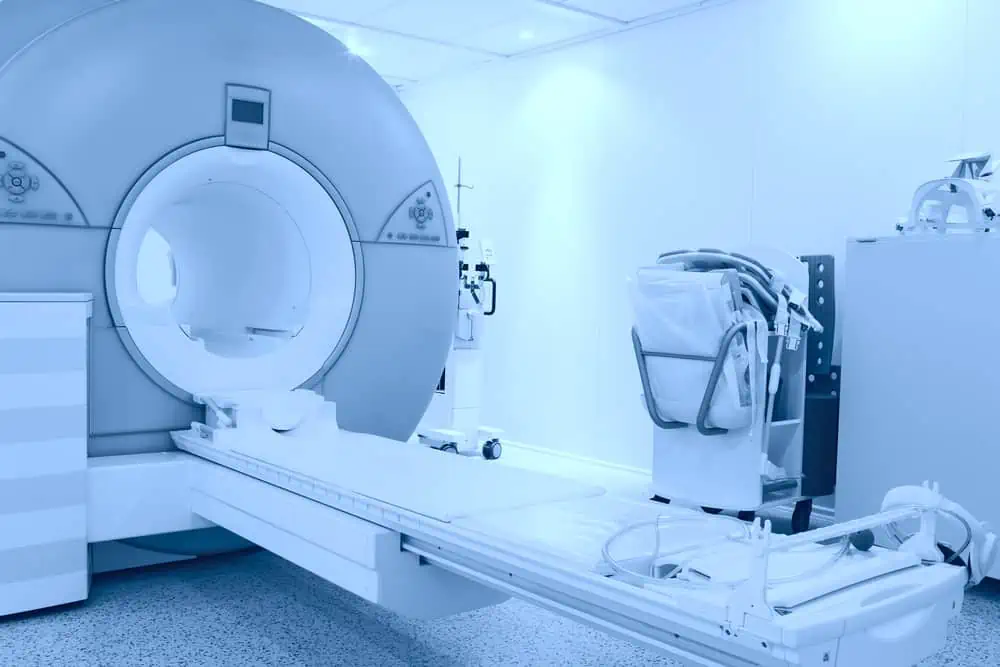
An MRI machine looks like a large tube. During the procedure, you’re moved into the machine on a sliding platform, which can be very claustrophobic for some. While it may seem comfortable to lie down, it’s not a great time to take a nap, as the MRI scanner is very loud while taking images.
You can speak with your MRI technician about using earplugs or headphones during the MRI scan or even speak with your doctor about a mild sedative to ease anxiety if that’s appropriate.
Not everyone can have an MRI for certain reasons. Since MRI is a big magnet, people with pacemakers, cochlear implants, other metal implanted devices, and more are not able to have this type of scan.
These contraindications will be listed in your consent before imaging, so make sure to read them thoroughly to avoid adverse issues or harm.
How is an MRI different from a CT?
A CT (computed tomography) scan is different from an MRI. CT scans take a fast series of X-ray pictures, which are assembled together with digital computer technology to create detailed images of the area scanned.
Both CT scans and MRIs have different strengths and can visualize tissue slightly differently. CT scans are usually the first choice for imaging. MRIs are useful for certain diseases that a CT scan cannot detect.
CT scans are often a lot faster, and often completed within just a few minutes. An MRI can take 15-90 min to complete, depending on the tests ordered.
People with claustrophobia may find CT scans more tolerable since it’s more of a circle than a long tube.
Do I need an MRI for back pain?
Not as often as you would think. If you’re presenting with symptoms that are concerning for a more serious condition, then imaging may be one of the first things done.
However, if your presentation is consistent with musculoskeletal pain, for example, a muscle strain, bulging disc, or herniated disc, an MRI may not be necessary, especially in the earlier stages of your treatment.
It may be considered further down the line if you’re having a poor response to conservative efforts.
Red flags for back pain
Most of the time, back pain is not caused by a serious issue. Occasionally, back pain can be a sign of a more serious condition.
If you’re experiencing any of the following, don’t delay in getting care. Some can be unrelated or overlap with other explained reasons, but it’s best to get yourself checked. You may require an MRI or other medical imaging right away if you’re experiencing these symptoms.
- Unexplained back pain in young children or older adults
- Severe pain that is not relieved by prescription medication
- Atypical pain presentation
- Back pain accompanied by fever/chills
- Recent trauma, such as a fall
- A history of cancer, especially prostate, breast, lung, kidney, melanoma, ovarian, and thyroid
- Pain at night or pain at rest that doesn’t seem to improve by changing positions
- New onset bowel/bladder incontinence or inability to go to the bathroom
- Saddle anesthesia (loss of sensation in the area you would sit on a horse)
- New onset weakness or numbness in your legs
- New or sudden onset difficulty walking, difficulty with balance, or difficulty with coordination.
The problem with imaging
Unfortunately, imaging is not always the magical answer that everyone is looking for. A static picture often does not explain the whole story, and it’s important to view diagnostic imaging as a piece of the puzzle and not the end all be all.
Recent evidence suggests that 90-95% of uncomplicated low back pain does not require imaging and will improve with conservative treatment (patient education, exercise, physical therapy, chiropractic care, and pain management). In fact, having an MRI often does not lead to faster resolution of symptoms, better treatment, or better pain relief.
The mind is a very powerful thing. Many people have asymptomatic, normal age-related changes they were not aware of, and imaging can highlight these and cause additional fear and movement avoidance behavior. An example of this is when someone is told they “have the spine of an 80-year-old.” (There are plenty of 80-year-olds with great spines, by the way.)
This kind of information often causes people to avoid specific activities simply because they fear those activities will cause them pain or worsen their “bad back.” Over time, this can be very limiting and affect the quality of life and physical function. In reality, not moving causes more issues over time than smart movement.
Sometimes insurance companies will not approve an MRI until someone tries physical therapy for approximately 6 weeks. If this is the case, it’s important to give PT a fair effort, including attending all appointments and performing your prescribed home exercises.
In order to see improvements in pain, strength, and mobility, physical therapy takes at least a few weeks of solid consistency to see improvement. It’s important to put in some good-faith effort and not simply “check the box” to get your imaging. Who knows, you may even wind up feeling better by then.
Imaging also may not be covered or fully covered, with high co-pays or deductibles left over for you to pay out of pocket. This can sting even harder if your MRI comes up with nothing useful.
Related read: 13 Things To Avoid When You Have Sciatica
Pain level often doesn’t match up with imaging findings
An interesting finding that is incredibly frustrating for people is that pain levels frequently don’t match up with imaging results, meaning you could end up not receiving any additional information after a scan.
There are three concepts in new research that are changing the way healthcare providers treat pain. This is also helpful information for patients in understanding pain.
The first concept is that pain is not a signal originating from a particular bodily tissue. While there are localized chemical processes at the site of an injury (such as tissue damage and repair), the pain response is ultimately controlled by the nervous system and can have far-reaching effects throughout the entire body.
Essentially, experiencing pain is not as much about what’s injured but rather how the nervous system interprets and responds to the injury. There are always multiple factors at play, and pain can exist without injury or visible tissue damage.
Second, pain is not an accurate measure of tissue damage. When we have a lot of pain, we naturally think something is wrong. New findings suggest that the severity of an injury doesn’t necessarily correlate with the amount of pain someone experiences.
This accounts for differences in pain tolerance between people with a similar type of injury. An interesting finding is that pain frequently doesn’t match up with the amount of tissue damage on imaging, leaving people frustrated and confused when their MRI doesn’t explain the cause of their pain.
Lastly, the plasticity of the nervous system means that the nervous system itself is a viable target for the treatment of pain. Plasticity refers to the ability to adapt and change from experience and stimuli.
We can’t ignore the nervous system’s role in how we experience pain. Targeting the nervous system in various ways, including movement, strengthening, and mind-body techniques, can help the nervous system adapt. (Parker R and Madden V, 2020)
The best part is, you’re never too old to benefit from these interventions, but you do need to approach healing with a positive mindset.
How will my physical therapist know what to do if I don’t have an MRI?
As humans, it feels good when we have more information and can put a face to a name regarding our pain; however, having an MRI often does not change your physical therapy plan.
Different diagnoses present differently, and a good doctor and physical therapist should be able to examine you and have a better understanding of what’s going on and make recommendations accordingly.
It’s when presentations don’t follow specific patterns, or red flags are present, that there is more cause for concern and further testing.
Physical therapists are trained in the diagnosis and treatment of musculoskeletal injuries, including knowing when to refer someone to a physician for further workup if things seem concerning.
At your first physical therapy visit, your therapist will do a thorough evaluation and physical examination to assess your specific issues and limitations and design a plan for you.
The bottom line is that having an MRI or not doesn’t change how you’re feeling or presenting, and you’ll still need to work on regaining normal mobility and function.
You know your body best
At the end of the day, it’s your job as the patient to be your own advocate for your care, and sometimes that means pushing for what you need.
As advanced as modern medicine is, some things can still fall through the cracks, so if you feel like something isn’t right (especially if you’re having red-flag symptoms), push for what you need. This may include getting multiple opinions, especially if you get the sense that your concerns are not being taken seriously.
Take good notes on your symptoms, and be sure to articulate them clearly to your providers. Healthcare providers are not mindreaders, and only you know what your body feels like. The more detail you can provide, the better care you’ll receive.
A good provider also should be explaining to you why or why not imaging is warranted and make sure you understand and are comfortable with the plan.
Wrapping up
Most back pain that is musculoskeletal in nature does not require an MRI and will improve with conservative treatment and time.
If your pain persists or presents with other red flags, an MRI is likely to be done sooner than later to rule out more serious conditions.
To get the best care possible, stay informed about your condition and any treatment or tests you receive and advocate for yourself. Don’t be afraid to seek a second opinion if you feel like you’re not getting the care you deserve.
References
Ghadimi M, Sapra A. Magnetic Resonance Imaging Contraindications. [Updated 2022 May 8]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2023 Jan-. Available from: https://www.ncbi.nlm.nih.gov/books/NBK551669/
Hall AM, Aubrey-Bassler K, Thorne B, Maher CG. Do not routinely offer imaging for uncomplicated low back pain. BMJ. 2021 Feb 12;372:n291. doi: 10.1136/bmj.n291. PMID: 33579691; PMCID: PMC8023332.
Parker R, Madden VJ. State of the art: What have the pain sciences brought to physiotherapy? S Afr J Physiother. 2020 Feb 24;76(1):1390. doi: 10.4102/sajp.v76i1.1390. PMID: 32161828; PMCID: PMC7059532.