This post may contain affiliate links. If you click through a link and make a purchase, I may receive a commission at no additional cost to you. As an Amazon Associate, I earn from qualifying purchases. Read the full disclosure here.
Sacroiliac pain can be a frustrating experience when pain is waiting for you at every step.
A big part of getting better is quickly is understanding what not to do to avoid constant flare-ups.
But what aggravates sacroiliac joint pain?
This article will take you through the basics of SI joint pain and explain what to avoid so you can start feeling better fast.
Disclaimer: This content is for educational purposes and is not medical advice. Read the full disclaimer.
What is the sacroiliac joint?
The SI joint can seem complicated and mysterious, so let’s break it down.
The pelvic girdle is three major bones connected together to include a right and left coxal bone and sacrum. The coxal bone is sometimes called the pelvic bone or the hip bone or pelvic bone because it houses the hip socket.
The sits-bone (ischial tuberosity) is a region of the coxal bone.
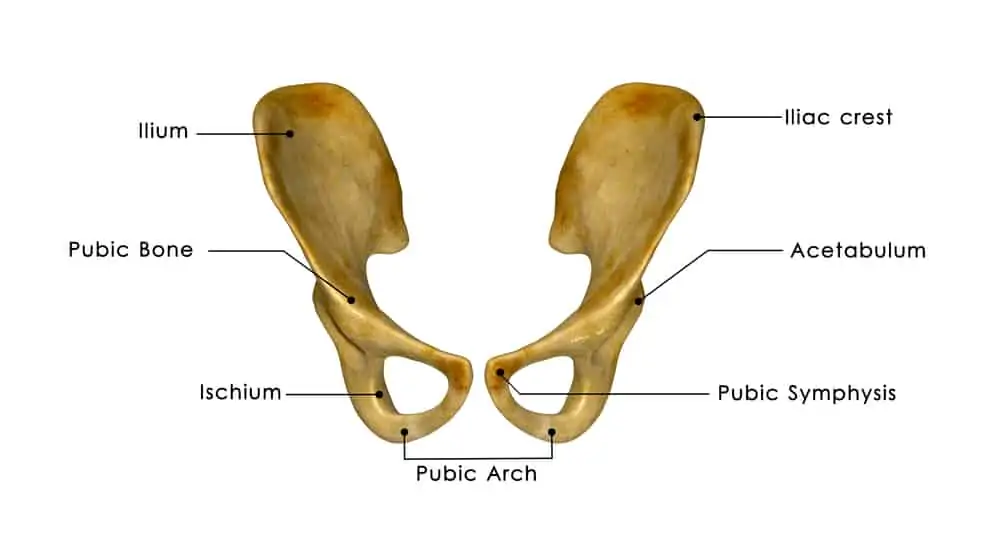
The sacrum connects the two coxal bones in the back and the pubic symphysis (a thick piece of cartilage) connects the bones in the front. The coccyx (tailbone) sits at the bottom tip of the sacrum.
The sacroiliac joint (often referred to as the SI joint for short) is a bilateral joint, with a right and left SI joint on each side of the sacrum.
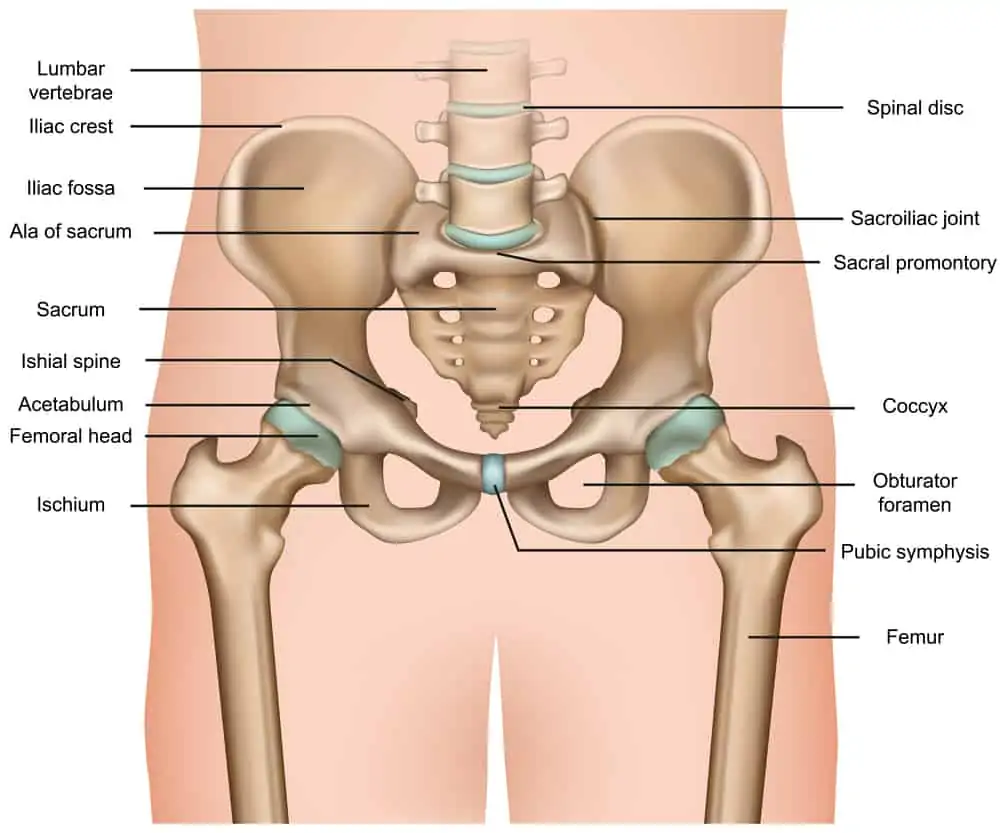
The SI joint is extremely stable at the crossroads of the hips and lower back and is surrounded by some of the strongest and most powerful muscles of the body.
The primary role of the SI joint is to transfer force and absorb shock between the lower body and the lumbar spine.
There has long been debate on whether or not the SI joint has any mobility. Most medical professionals agree that mobility is limited to only a few degrees due to the joint structure and reinforcement by thick ligaments.
What causes sacroiliac joint pain?
SI joint pain is more common in women and is estimated to be present in 15-30% of low back pain cases each year.
This is likely due to the difference in pelvic structure and mechanics, changing the stress and load through the joints, as well as hormones that increase ligamentous laxity.
Possible causes of SI joint pain:
- Injury (repetitive strain or traumatic)
- Pregnancy
- Hypermobility
- Referred pain from the lumbar spine
- Arthritis
Compared to other joints of the body, no muscles specifically act to move the SI joint, but several large muscles from the hip joint and lower back cross or attach near the area and can indirectly affect forces through the sacrum.
Symptoms of SI joint dysfunction
Sacroiliac dysfunction is generally thought to be caused by either a lack of motion (hypo-mobile) or too much motion (hyper-mobile).
This can result from repetitive strain over time or a single traumatic injury such as a fall or direct force.
Due to the structure of the SI joint and how it fits into the pelvis, the amount of motion is very little but can have a painful impact on the joint and surrounding tissues.
Remember, the main role of the SI joint is to stabilize and transfer forces between the lower body and lumbar spine. If this kinetic chain is disrupted, it can have far-reaching effects.
Symptoms of SI joint dysfunction can include:
- Lower back pain, hip pain, and/or buttock pain
- Pain that increases with movement, especially asymmetric activities like climbing stairs or prolonged sitting
- Sharp or dull pain in the area of the SI joint
- Sciatic-like symptoms
- May overlap with lumbar spine pain or be confused with lumbar radicular pain
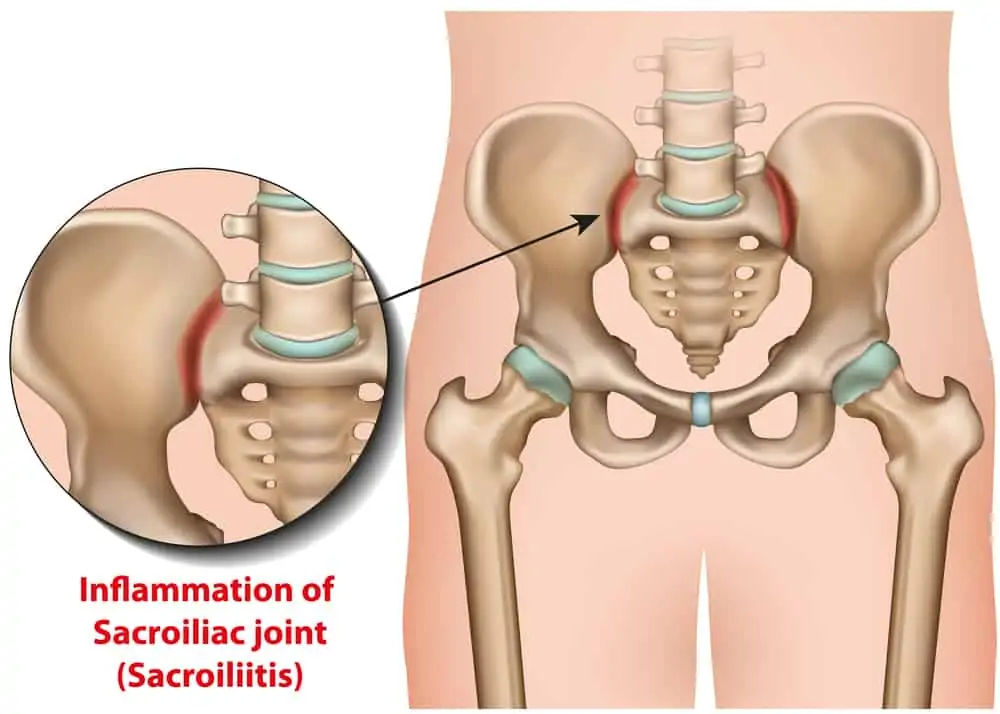
How can you tell lower back pain from SIJ dysfunction?
It can be tricky. The SI joint is often overlooked as a source of pain or can mimic other conditions that are more common.
Your doctor (especially someone with experience in orthopedics and the spine) and physical therapist can perform various low back and hip tests to attempt to reproduce your symptoms.
If several specific tests are positive, there may be some SI joint involvement.
Keep in mind, it’s also possible to have more than one issue at a time.
Finding the proper diagnosis is sometimes a work in progress. An MRI may be able to detect joint inflammation or may provide no useful information at all. Imaging frequently doesn’t line up with pain levels.
Keeping close track of when your symptoms occur (such as with specific activities) can help establish a diagnosis.
What aggravates sacroiliac joint pain?
A big part of getting better quickly is understanding what not to do to avoid constant flare-ups.
Here is a list of some everyday activities that can aggravate SI joint dysfunction.
Are any of these activities increasing your pain?
Sitting, especially with crossed legs
If the SI joint is already cranky, sitting in a slumped position, crossing your legs, or sitting with one leg underneath your hips may increase your pain.
Try to optimize your sitting posture by keeping your feet flat on the floor and using a lumbar support pillow to maintain good alignment in the lower spine.
For more tips on how to avoid slouching at your desk, check out this article.
Climbing stairs
A painful SI joint will be sensitive toward asymmetrical activities.
An example of this is climbing stairs, where force is transferred through the pelvis one leg at a time.
If your SI joint is particularly painful, try stepping up/down the stairs one step at a time instead of step-over-step.
The larger the step, the more strain and, therefore, more painful.
Taking shorter strides while walking can also help limit aggravation to the area.
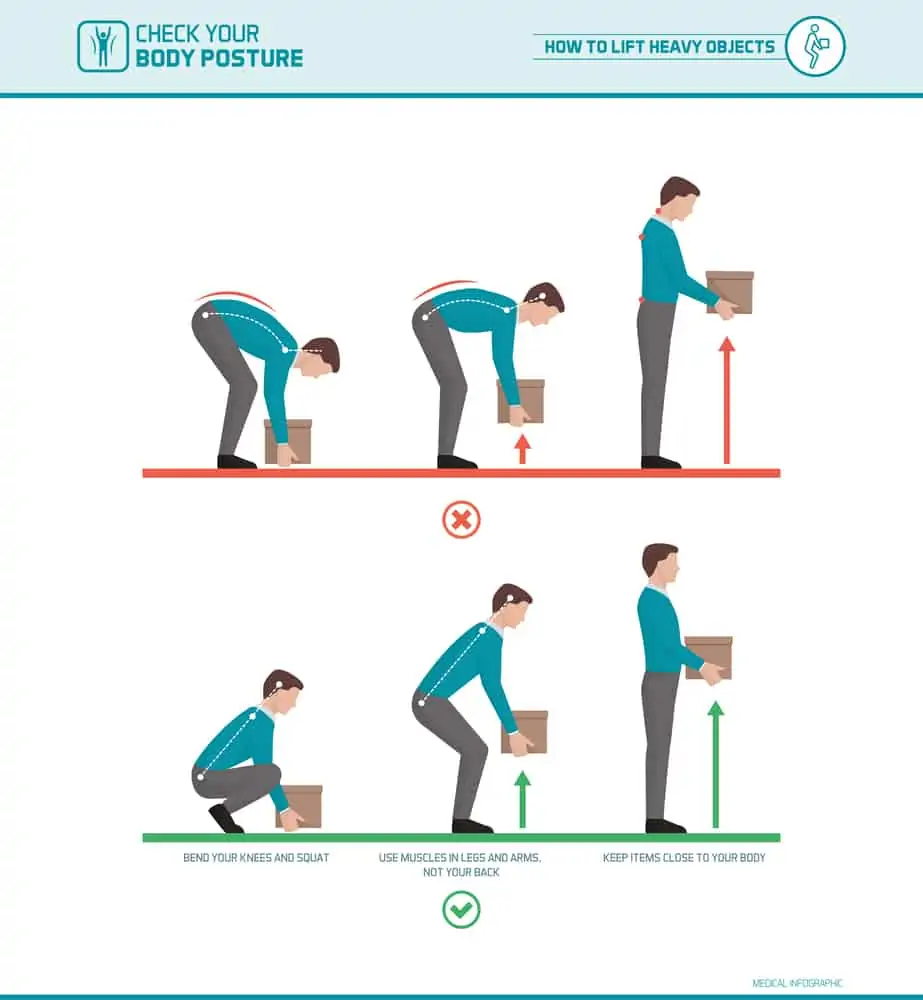
Lifting and twisting
Everyday home activities such as shoveling snow, gardening, or house cleaning activities that involve lifting and twisting can aggravate SI joint dysfunction.
To minimize discomfort, use good body mechanics and move one step at a time, separating lifting and twisting to ensure you have a stable base.
Asymmetrical exercises
Asymmetrical exercises (performing one side at a time) can add additional stress to the SI joint.
Exercises such as lunges, step-ups, or single-leg deadlifts are examples of asymmetrical exercises.
Stick with neutral/symmetrical exercises such as modified squats, bridges, bilateral rows, and pull-downs as you heal.
*Heads up – popular machines at the gym for hips are abduction/adduction machines. Though this technically follows the symmetrical rule because both sides are working simultaneously, the motions have the potential to compress or gap the SI joint and cause additional pain.*
To work these muscles with less force, try abduction with a band around the knees in bridge or adductor ball squeeze with a bridge to modify as you’re healing.
High impact activities or heavy weight lifting
Running, jumping, and other high-level impact activities can increase the force through the joint and worsen symptoms.
Lifting heavy weights, especially asymmetric exercises, can increase force through the SI joint and result in pain.
Certain yoga poses
Yoga is often thought of as a gentle exercise, but it depends on the style of yoga.
A cranky SI joint can be sensitive to many movements, even in gentle practices.
Examples are high lunge, warriors, forward folds, backbends, twists, and hip opening poses.
How you respond to these poses depends on what type of SI joint dysfunction you have.
To avoid aggravating your symptoms, adjust the width/angle of your feet and choose lighter versions of poses to avoid straining the joint.
Some examples are:
- Supine figure 4 stretch is more gentle than pigeon
- Sphinx is more gentle on the SI joint than cobra or upward facing dog
- Try placing your hands on blocks in forward fold to modify the range of motion
- Swap in cat-cow to a sun salutation instead of chaturanga and upward facing dog
Are there specific SI joint exercises?
Physical therapy can be helpful in providing safe exercises for SI pain. A combination of stretching and hip strengthening exercises is usually prescribed.
Here’s an interesting paper with promising results for SI pain (even chronic SI joint pain) that physical therapist Ryan Whelton created.
It includes a simple four-step exercise protocol to reduce SI joint pain.
It’s worth noting that for this protocol to be beneficial, a proper diagnosis needs to be established. If your issue isn’t SI joint-related, they may not be of much help.
Getting SI joint pain relief
When you have SI joint pain, you’re always looking for ways to feel better fast.
You might be wondering if modalities like ice/heat or even TENS will help your pain.
These treatments can be helpful in the short term, but it’s important to remember that they only provide temporary relief and are not “fixing” anything.
You can read more about TENS units for pain relief in this article.
Passive treatments (treatments requiring no effort on your part) are OK to use in conjunction with treatment, but not as the only treatment.
To truly get rid of your pain and get back to normal activities, it’s essential to have a comprehensive evaluation, work with your doctor and physical therapist to improve strength and stability, and establish safe ways to get moving again.
Do SI belts work?
A sacroiliac belt or pelvic belt is different than a lumbar spine brace.
An SI belt is a stabilization belt worn lower on the hips to offer additional external stability to the SI joint and are often used during pregnancy and post-partum.
Evidence is mixed on the effectiveness of stability belts, especially whether or not a decrease in pain is attributed to improved muscle activation or a psychological sense of security.
Hammer N et al. designed a case-control study to compare clinical and functional data of patients with SI joint pain vs. healthy subjects to assess the effects of an SI belt on pain.
The study concluded a positive effect on SI joint pain and improved steadiness with walking. Adding an SI belt may be a low-risk treatment option as part of a comprehensive plan.
Caution with belts and braces as they can provide a false sense of security and lead you to continue aggravating activities which can slow your progress. They shouldn’t be thought of as a permanent solution.
It’s also worth noting that SI belts work best when the issue is instability, otherwise they likely won’t provide any benefit.
The best way to determine if an SI belt is right for you is to discuss your case with your healthcare providers.
Wrapping up
Sacroiliac joint pain can be frustrating and confusing.
Understanding how this area of the body works can help you make smart choices about your movement to avoid aggravating the SI area while you heal.
Be sure to get checked out by the appropriate health care professional to establish the right diagnosis and treatment plan for you.
References
Barros G, McGrath L, Gelfenbeyn M. Sacroiliac Joint Dysfunction in Patients With Low Back Pain. Fed Pract. 2019;36(8):370-375.
Hammer N, Möbius R, Schleifenbaum S, et al. Pelvic Belt Effects on Health Outcomes and Functional Parameters of Patients with Sacroiliac Joint Pain [published correction appears in PLoS One. 2015;10(10):e0140090]. PLoS One. 2015;10(8):e0136375. Published 2015 Aug 25. doi:10.1371/journal.pone.0136375Barros G, McGrath L, Gelfenbeyn M. Sacroiliac Joint Dysfunction in Patients With Low Back Pain. Fed Pract. 2019;36(8):370-375.
Kiapour A, Joukar A, Elgafy H, Erbulut DU, Agarwal AK, Goel VK. Biomechanics of the Sacroiliac Joint: Anatomy, Function, Biomechanics, Sexual Dimorphism, and Causes of Pain. Int J Spine Surg. 2020;14(Suppl 1):3-13. Published 2020 Feb 10. doi:10.14444/6077







Thank you, Maura, for another informative article. I always find good advice in your postings.
Thanks for reading Karen!